What to Expect During Recovery from Gynecomastia Surgery
After Gynecomastia:
What To Expect In the Days, Weeks, and Months After Male Breast Reduction Surgery
By Dr Mordcai Blau
Jump To:
After Gynecomastia:
What To Expect In the Days, Weeks, and Months After Male Breast Reduction Surgery
By Dr Mordcai Blau
Swelling and bruising are normal phenomena after surgery. Bruising (ecchymosis) can appear in various degrees, ranging from minimal to massive. It can be confined to the breast area or expand to the chest and abdomen. Bruising can appear as bright red, black, blue, purple, or a combination of colors. It will increase in intensity over the first 3-4 days, and then will diminish and become yellowish for another week or so. The discoloration will usually disappear in 2-3 weeks. During this time sun exposure is absolutely forbidden due to the possibility of permanent skin discoloration.
Swelling can be diffused or localized. Diffuse swelling can be treated by cold compress for the first 2 days and warm compress thereafter. Localized or minimal swelling is asymptomatic and no treatment is required.
Severe swelling can sometimes occur after surgery. The following are the forms of severe swelling:
Hematoma: is an acute collection or accumulation of fresh blood that can happen within the first 10 days post surgery, most commonly in the first 3 days, and causes an extreme, painful swelling of the breast. The breast feels hard and tender to the touch. There usually is blood on the gauze. Most often it is unilateral although it can be bilateral.
Severe cases require urgent treatment, and next day treatment is suitable in less severe cases.
Treatment can be of two varieties. In open treatment, the operating wound has to be opened and the blood clot evacuated through hemostasis (stopping the bleeding). Another treatment is done by puncture. Using a large gage needle under local anesthesia, the blood clot and partial operating wounds are evacuated by separation and drainage of the blood. Sometimes this treatment is only available when the blood clot liquefies within 2-10 days.
Seroma: is a combination of body fluid and liquid blood products. It is very liquidy with low viscosity and appears as red-orange color. It can easily be evacuated by a large gage syringe puncture under local anesthesia. The seroma usually needs a few evacuations 2-3 times over the first week or two after Gynecomastia surgery.
Pressure dressing is required for 3-5 days after evacuation of the hematoma or seroma.
When the correct treatment is done, late side effects such as excess skin, infection and discoloration are rare. Preventative measures to avoid bleeding and prevent hematoma formations include:
The first 3 post op days are the most critical time for the Gynecomastia patient. He must be in full rest at home (not necessarily on bed rest; sitting and watching TV or having meals in the kitchen are permissible). Going out to the mall for a few hours is forbidden. Movements of the waist and elbow are ok but the vigorous movements of the shoulder joints have to be restricted (curtailed) for the first few days. Lateral arm movements are generally permitted, but it is forbidden to lift the arms vertically. There are many variables and you should consult a board-certified plastic surgeon for more details.
The following are only general instructions (every patient has different needs): Prolonged walking and jogging can be done after 2 weeks. More extensive exercise including leg and arm exercises (not including shoulder joint and arm movements that use the pectoralis muscle) can be started in 2-½ – 3 weeks and intensify over the next 2 weeks. Chest (mainly weight lifting) and intensive abdominal & back exercises are generally permissible after 4-5 weeks. Sex is not recommended for the first 7-10 days.
Every surgeon has his own experience, and the type of dressing is up to the surgeon. Most surgeons use some kind of dressing or compression garments like vests, ace bandage, elastic bandage and other types of dressings.
The length of time the dressings are used varies from a few days to a few months. Personally, for my patients I determine the length of time the compression dressing should be used according to the severity of the surgery and the amount of bleeding and swelling. I always leave it for at least 5 days. It is at this time that I usually remove the sutures. Should the patient’s chest be very swollen, and if seroma or hematoma is present, I will apply new compression dressing for an additional 5 days. After this next 5-day period, I examine the patient again and usually remove the compression dressing. Only in very few circumstances will I leave it for additional time. According to my experience any compression dressing is most effective in the first week after surgery.
As after any surgery, exposure to direct sun or tanning should be avoided for about 6 weeks, until ecchymosis (bruising) and a fair amount of swelling subsides.
The main reason is that the sun rays will prolong the swelling and may cause the discoloration to be permanent. Sun exposure in the early stages can cause the scar to become more noticeable later due to pigmentation.
Therefore, when going out on a hot summer day with light clothing or no shirt, a sun block of at least 30 SPF should be applied for the first few months.
In my 25 years of experience with male breast reduction surgery I have found that typically the best location for the scar is periareolar (the lower lateral part under the areola) with a length of about one inch.
Most other scar locations will cause it to appear more conspicuous. After performing thousands of male breast reductions I have observed scars on the upper areola, sides of the areola, inside the areola, and many others. Scars done in the axilla (armpit) are not effective for me because I cannot excise the entire gland from this site.
“Domate incisions” around the entire areola are rarely necessary and should be avoided as a rule due to the possible thick, irregular, and prominent scarring it often causes.
Mederma, scar guard and other scar reduction creams should be used only as directed by your experienced board-certified plastic surgeon. In my experience they are helpful only in certain conditions (tendency for hypertrophic keloid scars) and are used as a preventive measure and post operatively. In my opinion it is unnecessary to use these products with the majority of Gynecomastia patients.
Many male breast reduction patients develop post op inner scars in the surgical sites. It can be felt as a hard “Donut” surrounding the nipple or lumps behind the nipple areola complex extending medially and laterally (toward the armpit)
This hard inner scar phenomenon is normal and appears very frequently. At times it can be mistaken as an incomplete excision of the glandular tissue. Fortunately, in my experience inner scars will disappear within a few months after the surgery. Rarely, there may be a need for scar excision. This is due to the rare tendency to produce an abundant amount of scar tissue while healing.
Should there be a need for a major breast reduction in those patients that have extremely large breast (C or D-cup compared to women’s breast sizes) I may perform a superior pedical breast reduction (Weiner technique), or sometimes an inferior, oblique, or medial pedical. The problem in such an extensive breast reduction is the scarring that extends from around the areola to an inverted T (a vertical incision and then horizontal incision that is placed in the Infra mammary crease). I found, using my own technique modifications, that the shorter the vertical component, the better the overall final appearance. In some cases an injection of Kenelog, a kind of cortisone, may be used to improve hypertrophic scars (keloid). This is not often necessary.
As with most surgeries there may be an area around the operating wound that will suffer a temporary decrease in sensation. From my experience it happens more often in patients with enlarged male breast that also require significant liposuction. Most male patients find the temporary loss of sensation to be insignificant. Sensation returns after a year for most patients.
There is a phenomenon of spontaneous shrinking of the entire areola after the male breast reduction surgery. The diameter of the areola will decrease 10-50% from the original size. This occurs in most patients when significant amounts of glandular tissue are removed. Therefore when a significant amount of breast tissue is removed over 90% of patients will experience this natural phenomenon of a spontaneous decrease in the areolas diameter. This is another reason why I rarely employ excision around the areola.
The purpose of massaging the breast post operatively is to break up and reduce the bulk of the scar tissue.
Massage can done with the palm of the hand or between the thumb and the other fingers. Gentle massage is superior to rough massage and it should not be painful, just tender. It should not be started in the first week. I want to stress that massage after gynecomastia is not necessary in many cases. It can be helpful with the temporary conditions of scarring and swelling but does not improve remaining glandular or adipose tissue. In other words it is not a solution to get rid of tissue that was not excised during the male breast reduction procedure. For scar tissue, the injection of kenelog is much more effective.
Gynecomastia patients that have severe medical problems will need clearance from their physicians.
The list of medications to be avoided is sent to the patient with our pre-surgical booklet and includes blood thinners like aspirin and other medications. All nutritional supplements should be avoided for the same reason. Alcohol consumption should be decreased starting one week prior to surgery and one-week post surgery and should be totally avoided a few days before and after surgery. All steroids should be stopped two weeks prior and two weeks post surgery. Our patients are provided with a detailed guide listing everything that must be avoided.
We assist our patients that are traveling from other countries, states and cities with their lodging arrangements by providing hotel options near our facility.
Since our location is in the heart of White Plains there are several convenient lodging places two blocks from the office.
Dr. Blau may begin the correspondence over the internet and give an online consultation, but the patient has to be examined a day prior to surgery for the final determination.
The patient has to provide us with photos and a detailed medical history and will get a comprehensive booklet that is addressed to his specific needs. After the surgery patients will remain in the office facility until they are completely stable and then one of our staff members will take him to his lodging place.
Depression of the areola is extremely uncommon in our patients but may occur post surgery and will usually subside within 3-6 months. Should the problem persist after 6-12 months there may be a need for adipose transfer from the abdominal area that is a pretty simple procedure generally performed under local anesthesia.
So far, after thousands of Gynecomastia cases, we have never had the need to perform this procedure. I attribute this to my “Natural Blend Technique” that emphasizes proportionality and the needs of each individual patient.
In some patients with diminished elasticity (more common in elderly patients) there may be excess skin or skin creases that are more noticeable post op. Most of those creases will persist for 6-12 months and then diminish significantly, and the loose skin usually tightens.
The 1st follow-up visit will usually occur after 5-7 days post op. This is an important visit and the sutures will be removed at this time. Should there be a drain it may be removed at the same time if the discharge is diminished or disappears.
The compression dressing will be removed, depending on the healing of the operating wound and the presence of edema (swelling or fluid). In some cases the compression dressing will be reapplied for an additional 5 days.
Usually patients are not put on antibiotics, and only if there are any signs of infection or in complex cases will patients be put on antibiotics.
Neosporin and other antibiotic ointments are applied to the wound only as required (as superficial skin slough or slightly opened wounds).
Living a life free of Gynecomastia is the ultimate payoff for most male breast reduction patients. The benefits are well known. However, it is important to be educated about what the surgery entails and what the post-operative period will be like. We hope this guide has given you some insights into this critical period.
Remember to speak with a board certified plastic surgeon for more specific information.
Photos Courtesy of Dr. Elizabeth Zellner and Dr. Mordcai Blau, M.D., P.C. ~ Individual results may vary.
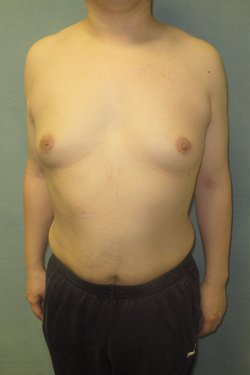
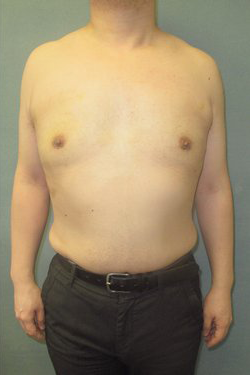
I was recently a patient of Dr. Blau. I had gynecomastia surgery done by him back in December 2013. I don’t think the surgery could have been more successful. After tons of research beforehand, I wasn’t able to find a more qualified surgeon, so I went ahead and had him perform the procedure. As a person who had and now doesn’t have gynecomastia I will tell you right now it was worth every penny. Now I have more confidence in my body and I can actually wear whatever I want now without thinking twice.(if you’re reading this you understand) From Doctor Blau’s professionalism, friendliness, and steady hands the entire process went about smoothly and now 4 months later I have no regrets. I feel that the results speak for themselves. The recovery was relatively quick; few days with a bandage, stitches come off by themselves, and Dr. Blau removing any extra fluid; I was back to working out in 2 and a half weeks and there’s pretty much no scar. If you’re looking to get a gynecomastia procedure done by a more than qualified surgeon who cares and results matter to you look no further than Doctor Blau, I know i don’t regret it.
By W.S.