Adolescent Male Breast Reduction
Gynecomastia is a significant psychological and social problem for adolescents and may leave a negative impact that carries on into adulthood. Protruding breasts in young males often leads to teasing from peers, and usually, the adolescent will avoid dealing with the condition. Behavior frequently includes hiding the chest in public, such as swimming, taking their shirt off, or withdrawing from others.
Dr. Mordcai Blau and Dr. Elizabeth Zellner area board-certified plastic surgeons specializing in gynecomastia and offers adolescent male breast reduction surgery in White Plains, NY.
About Gynecomastia in Adolescents
Congenital or Hereditary Gynecomastia is usually evident in boys between the ages of 10 to 12. Thirty to sixty percent of young boys suffer from large male breasts, and as many as 30% may live with enlarged male breasts for the rest of their lives.
Gynecomastia in teenagers may also occur as a result of obesity and less often for hormonal reasons, such as Klinefelter Syndrome and testicular tumors. In many cases, though, no specific cause of gynecomastia can be found.
In true gynecomastia, the breast enlargement is due to glandular breast tissue (mammary tissue), and in pseudogynecomastia, excess adipose tissue is the cause of the enlarged chest. It is marked by the diffuse fatty tissue infiltration of the breast & axillary (armpit) areas.
In pseudogynecomastia cases, diet and exercise may be advised before considering surgical procedures. In many adolescent gynecomastia cases, glandular and fat tissues are present. In these cases, the adolescent develops larger-than-normal deposits of glandular and adipose tissue, and these tissues may be permanent.
Dr. Blau and Dr. Zellner observe that there may be residual glandular tissue in severe cases. In many other cases involving tubular or saggy breasts, gynecomastia may remain behind the nipple-areola complex well into adulthood and is mostly permanent.
Your Adolescent Male Breast Reduction will be performed in Dr. Elizabeth Zellner's surgery center located in White Plains, NY.
How Does Adolescent Male Breast Reduction Help Patients?
Adolescent gynecomastia surgery provides both physical and psychological relief for young males dealing with enlarged breast tissue. This condition often causes emotional distress, impacting a teenager’s self-image, confidence, and social interactions. The surgery effectively addresses these concerns by:
- Reducing Physical Discomfort: Surgery removes the excess glandular and fat tissue, alleviating symptoms like physical discomfort and tenderness in the chest area.
- Enhancing Confidence and Self-Esteem: This procedure can help adolescents feel more comfortable in their appearance, reducing anxiety and self-consciousness in social situations.
- Offering Long-Lasting Results: Most patients experience permanent results from the surgery, allowing them to confidently move forward as they transition into adulthood.
By addressing both the physical and emotional aspects of gynecomastia, this procedure can significantly improve a young patient’s quality of life.
Ideal Candidates for Adolescent Male Breast Reduction
The ideal candidate for adolescent gynecomastia surgery is an adolescent who has experienced persistent breast enlargement for over two years without improvement. Typically, candidates are emotionally mature enough to understand the procedure and have realistic expectations about the results.
Other criteria include:
- Candidates should be in good overall health with no underlying conditions that could complicate surgery or recovery.
- The patient should have ideally completed most of his pubertal growth to avoid further hormonal changes that could affect the chest.
- Patients who have not responded to conservative approaches like diet and exercise, particularly in cases of pseudogynecomastia, where fat tissue is the main contributor.
Dr. Blau and Dr. Zellner will conduct a thorough consultation to determine if the patient is an appropriate candidate for gynecomastia surgery, ensuring that the decision to proceed is well-informed.
Procedure Details
Gynecomastia surgery mainly consists of male breast reduction surgery. In the opinion of Dr. Blau and Dr. Zellner, there is an obvious indication that male breast surgery should be performed in selective cases.
For adolescents with persistent or severe gynecomastia, male breast reduction surgery is a viable option. The procedure typically involves removing excess glandular tissue and fat from the chest via liposuction. In more severe cases, the procedure will include tightening the skin to achieve a more natural contour.
Dr. Blau and Dr. Zellner customizes each procedure based on the individual’s anatomy and needs, ensuring the best possible outcome.
Results
The following adolescent male breast reduction before-and-after photos will give you a sense of the results Dr. Blau and Dr. Zellner have achieved in teenage gynecomastia surgery. However, each patient is unique, and previous results do not guarantee individual outcomes.
Photos Courtesy of Dr. Elizabeth Zellner and Dr. Mordcai Blau, M.D., P.C. ~ Individual results may vary.
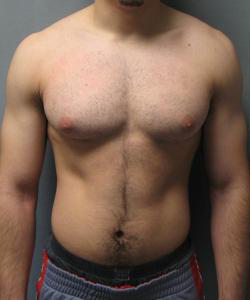
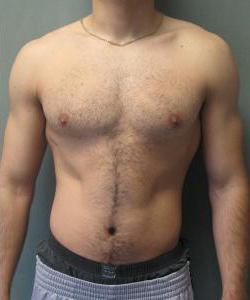
Adolescents must follow specific aftercare instructions, including wearing compression garments to support healing and attending follow-up appointments. Swelling and bruising are common but should subside within a few weeks. Most patients see significant improvement in the chest’s appearance and report a boost in emotional well-being as they gain confidence in their body.
Full results are typically visible after several months as the body heals completely. Our guide to gynecomastia recovery has more information, especially for teenagers.
Cost of Adolescent Male Breast Reduction
The cost breakdown of gynecomastia surgery includes medical tests, surgeon’s fees, the cost of anesthesia, hospital charges, and post-procedure garments. It is also affected by what type of procedure you will need and how long it will take to perform it. If it is unilateral gynecomastia, a condition affecting only one breast, it will cost around $6,900, but the cost will increase to $9,600 for bilateral gynecomastia.
A surgery for severe bilateral gynecomastia with sagging skin will cost $10,000 to $20,000.
You will know what procedure you will get after the consultation with Dr. Blau and Dr. Zellner.
Why Choose Dr. Blau and Dr. Zellner for Adolescent Male Breast Reduction?
Dr. Mordcai Blau is a leading expert in gynecomastia surgery with over 30 years of experience. He has developed a unique understanding of when early surgical intervention is necessary for adolescents. His personalized approach ensures that his young patients’ physical and emotional well-being are prioritized, making him a trusted choice for gynecomastia surgery in White Plains, New York. Working alongside him, Dr. Elizabeth Zellner has been personally trained by Dr. Blau and is fully versed in his advanced surgical techniques and philosophy of care. Through this direct mentorship, she upholds the same high standards of precision, safety, and patient-centered outcomes that define Dr. Blau’s approach.
A surgery for severe bilateral gynecomastia with sagging skin will cost $10,000 to $20,000.
You will know what procedure you will get after the consultation with Dr. Blau and Dr. Zellner.
Contact Us Today
After a significant number of adolescent patients, Dr. Blau and Dr. Zellner have developed a keen sense of when adolescent requires early surgical intervention.
If you know someone struggling with adolescent gynecomastia, let them know that Dr. Blau and Dr. Zellner are here to help. With his extensive experience and compassionate care, he can guide you and your loved one through every step of the process. Contact our office today to schedule a consultation in White Plains, NY, and take the first step toward restoring confidence.
Frequently Asked Questions
Is gynecomastia surgery safe for teens?
Yes, gynecomastia surgery is generally safe for teenagers when performed by an experienced surgeon like Dr. Blau and Dr. Zellner. They carefully evaluate each patient to determine if they are a good candidate for the procedure. Surgical risks will be discussed during the consultation to ensure informed decision-making.
How long does recovery take?
The recovery period usually lasts a few weeks, with most patients able to resume normal activities within one to two weeks. However, strenuous physical activity should be avoided for at least a month.
Will the results be permanent?
In most cases, the results of gynecomastia surgery are permanent. However, significant weight gain or hormonal imbalances can cause a recurrence of the condition.
Patient Testimonial
Dr. Blau – The artist of surgery! I developed gynecomastia during puberty and it affected my self confidence and self-esteem greatly. Being a three sport athlete in high school I trained frequently, but no matter how hard I trained I still suffered from “puffy nipples” / gynecomastia. As I grew older I always researched methods and treatments on how to correct the problem. Most of the articles I found said surgery was the best option. After researching plastic surgeons for approximately a year Dr. Blau was the man. I contacted his office and set up a consultation, before leaving I had my surgery booked. Dr. Blau is very passionate in what he does and wants his patients to be 100% satisfied with the results. I can say after 3 months Dr. Blau did a phenomenal job and I could not be happier with the results. He continues to follow up with his patients expressing his passion for what he does. If you are suffering from gynecomastia I would recommend Dr. Blau you will not be disappointed!
By R.B.





