Slimming The Arms (Brachioplasty)
Plastic Surgery Products
July 2006
Slimming the Arms
Mordcai Blau, MD
How to perform an arm lift for the massive-weight-loss patient—and how not to
 As massive weight loss, whether through bariatric surgery or intense diet and exercise regimens, becomes a more common occurrence, plastic surgeons are now seeing patients who need full-body lifts with higher frequency. Often, upper-arm surgery in these patients is considered part of a staged reconstruction.
As massive weight loss, whether through bariatric surgery or intense diet and exercise regimens, becomes a more common occurrence, plastic surgeons are now seeing patients who need full-body lifts with higher frequency. Often, upper-arm surgery in these patients is considered part of a staged reconstruction.
Most plastic surgeons would not perform full-body lifts (which involve thigh lifts, buttocks lifts, abdominoplasty, excision of excess skin in the back area, liposuction of the neck, and arm lifts) all at once. Indeed, that would be unsafe. As a result, in planning postbariatric surgery, the arm lift is just one of the stages that will eventually need to be addressed.
Each patient has a different preference. Some may prefer to address the stomach and back first; others may want to begin with their limbs. These are all expensive procedures, so patients will probably take their own finances into account when considering the order in which their reconstruction procedures should be performed.
According to statistics provided by the American Society of Aesthetic Plastic Surgery, there were 2,516 upper-arm-lift cases in the United States in 1997.1 Only 9 years later, there were 15,439 such cases—an increase of more than 500%. The frequency of lower-body lifts—including thigh lifts—has also increased significantly.
After massive weight loss, patients have a great deal of hanging, excess skin. Young patients, whose skin is more elastic, still require this surgery; the skin will not spring back because of the sheer amount of lost weight. Obviously, liposuction alone is not enough. These indications call for brachioplasty.
Brachioplasty with liposuction is much more prevalent in female patients. Whereas male patients ordinarily do not need liposuction in their arms or thighs, they may benefit from this procedure after massive weight loss.
Brachioplasty may be needed after any form of bariatric surgery, including the use of a constricting band around the stomach, stomach stapling, or partial stomach excision. In these patients, the skin has been extended for many years. They have lost a great deal of fat, but their skin remains flabby, requiring excision. This is common in the upper arm and axilla.
Ideally, a surgeon should treat only a patient who has achieved ideal weight postoperatively with the help of diet and exercise. I usually see patients about 1 year after bariatric surgery.
Of course, plastic surgeons should order all standard blood tests to ensure that hemoglobin and electrolyte levels are good. Because the skin tension in the arms and thighs is significant and the blood supply to the limbs is not as good as it is to the face, for example, scars may not heal as well.
Examination, Contraindications
When examining a patient, the surgeon should ask him or her to extend the arms forward and over the head to get a good visual impression of the arm fat and excess skin. At this point, the areas to be treated are marked.
During the surgical procedure, a small incision is made at the patient’s elbow. From this incision, liposuction will be done toward the axilla. In many upper-arm liposuction procedures, the surgeon will also have to perform liposuction at the axilla, both anteriorly and posteriorly. Many female patients with excess skin in their upper arms typically have excess skin in their axilla, so it is not uncommon to add skin excision in this area to the plan.
Before & After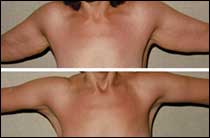
This patient was 35 years old at the time of the surgery. She had an arm reduction (excision) from the elbow to the axilla. By the time the postoperative photo was taken, 2 years later, the patient had lost 120 pounds, thanks to diet and exercise.
Contraindications include radical mastectomy with lymph-node excision. This is because the lymph nodes are missing in the axillae, so drainage in the upper arm may not be sufficient. In these cases, the patient is likely to experience constant edema of the arms.
Another condition to be aware of is hidradenitis, in which there is an inflammation of the sweat glands in the axilla. In this instance, lymphatic drainage is insufficient and, again, the surgeon should be extremely hesitant to perform liposuction or arm lifting.
Markings, Incision, and Surgery
any surgeons perform arm lifts using incisions in the medial part of the upper arm, which corresponds to the groove between the biceps and triceps. I prefer to put the scars in the midposterior or dorsal aspect of the upper arm (midline of the triceps muscle) because I have found that I get better results and less-noticeable scars. This scar will be more hidden, whether the arm is seen from the inner or outer aspect.
Before & After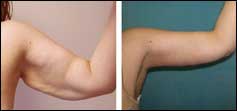
This is an example of a shorter excision. The patient lost 70 pounds prior to the arm-reduction surgery, during which extra tissue was removed between the middle of the upper arm to the axilla. The patient was 58 years old at the time of the surgery. The postoperative photo was taken 1 year later.
When making the incision in the brachial groove, the surgeon must be especially careful because this is not far from the brachial artery and the medial nerve. The incision should not be too deep to ensure that neither the artery nor the nerve will be injured. Because of this precaution, none of my patients has complained of any numbness.
Liposuction is usually performed with the use of tumescent anesthesia (injections of epinephrine, lidocaine, and bicarbonate) to minimize bleeding and inhibit pain. This solution should be injected into the upper arms. The optimal area for liposuction is usually the space under the triceps.
There are several degrees of excess skin. Some people have excess skin that extends from the elbow into the axilla. Other patients have excess skin only from the axilla to a point about halfway up the upper arm. Consequently, the extent of the procedure depends on the position of the excess skin and adipose tissue.
Before & After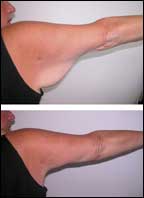
After undergoing bariatric surgery, the patient had an arm reduction. I excised excess skin from the patient’s elbow to the axilla. The scarring is visible only inferiorly—not at all laterally or medially. This patient was 23 years old at the time of the surgery and is 24 in the postoperative photo.
In instances in which it will be necessary for the excision to reach from the axilla to the elbow, the scar will be longer; however, it will be fairly straight. Some surgeons may prefer to break it up by performing a Z-plasty in the middle to reduce the scar’s overall length. Then, they will also have to excise excess skin when the axilla is reached, and a horizontal incision may result.
A plastic surgeon’s worst enemies in any brachioplasty are postoperative irregularities in the upper arm’s skin contour. The surgeon must be careful to take an equal amount from each arm and each subsection of the same arm.
Unfortunately, in combined excision–liposuction procedures, it is not uncommon to see a surgeon remove unequal amounts of excess skin and adipose tissue from various areas of the upper arm. Aesthetically, this is not an acceptable irregularity.
If this does occur, the surgeon may have to perform a second procedure that may include more excision and liposuction in those areas where excess fatty tissue or skin remains. The surgeon should keep this in mind and take care to keep the excision as symmetrical as possible.
The surgeon should always try to leave the shortest possible scar so that patients will feel comfortable wearing short-sleeved shirts. Unfortunately, this is not always possible. At a certain age, women who request liposuction and arm lifts may be more concerned with how they look when fully clothed. This is less true of younger patients, who often demand a less noticeable scar.
Before & After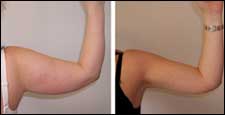
This 32-year-old patient had liposuction to remove approximately 150 mL of fat per arm. Arm reduction was done from the elbow to the axilla, in conjunction with liposuction in the thighs, stomach, back, and waist. The postoperative photo was taken 2 years later.
It will frequently be necessary to correct axillary adipose pads in women. These fat pads are most visible whenever the patient puts on a bra, which makes them bulge into the axilla. This area is often addressed as part of the upper-arm lift. Patients who are unhappy may blame it on these lumps, so it is essential for a symmetrical result in this area to be achieved.
When performing liposuction with excision in the upper arm, the surgeon must be careful not to use suction around the entire circumference of the arm because of the need to maintain lymphatic drainage. Circumferential liposuction may cause temporary or permanent swelling of the arm. Suction should never be applied to more than 75% of the arm; I prefer not to exceed a point halfway around the arm.
Should both arms be addressed concurrently? If the patient has someone to help him or her for a few days or a week, both arms can be corrected together. Otherwise, the surgeon should address each arm separately, and perform the procedures about 4 to 8 weeks apart.
Generally, I also perform excision and liposuction concurrently. In cases that involve younger patents with elastic skin, only liposuction may be sufficient. Still, in most cases, the patient has already been through massive weight loss, and it is harder to lose all the adipose tissue in this area; consequently, both liposuction and excision will be necessary.
Thigh Lifts and Hygiene
The number of thigh-lift procedures has dramatically increased over the past 5 years. For these procedures, infection becomes a greater concern than it is for upper-arm lifts. This is because a thigh lift is not done in a generally hygienic area. Obviously, people must use the bathroom; as a result, the area is more likely to become infected.
The likelihood of infection can be reduced using a regimen of antibiotics and regular cleaning. Therefore, it is imperative to give patients clear, direct instruction in how to clean the area after surgery; this should include the use of sponge baths. Arm-lift patients do not generally take antibiotics, but thigh-lift patients almost always do.
In the thigh lift, a vertical incision is made that goes from the groin to the popliteal area. I try to make this incision in the medial side of the thigh. There may sometimes be the need for a horizontal component at the top of the incision, as there is in the arm lift; in this case, it will be adjacent to the groin.
For these incisions, the surgeon should try to avoid extending the scar to areas where it may be very noticeable (for example, outside body creases). There may be patients in whom this sort of incision cannot be avoided, but the surgeon can typically keep the scar as short as possible. Instead of elongating the scar to those visible areas, the surgeon may just try to perform liposuction as well as possible.
Later, some small correction may be needed. Superiorly and posteriorly, these incisions can be made in the buttock crease; anteriorly, in the groin crease. These are good areas for concealing incisions. In some very minor cases, a horizontal or vertical incision may be sufficient, but it is commonly necessary to make both.
I have found that aesthetic surgery of the thighs—whether it involves liposuction, skin excision, or both—is much more common in women than in men. After massive weight loss, men usually have excess fat and skin only in their abdomen, back, and chest.
The quality of thigh-lift scars is unpredictable. If a patient has a history of keloids or hypertrophic scars in other areas, there may be an increased incidence of serious scarring in the limbs.
—MB
Postoperative Care
Postoperatively, I use a very light dressing. Using a heavy dressing will result in swelling of the arms and hands. I have used light dressings on my patients for the past 3 to 4 years and, in my experience, healing is usually good. Compression was common in the past, but is not needed.
After surgery, there is usually a red scar, and the patient will take some time to recover. Typically, the patient should keep the arm elevated for 1 to 2 weeks. Patients should reduce the use of the arm to a minimum for 10 to 14 days, performing only easy, light tasks. Patients will have to wait 6 weeks or longer to begin exercise and other strenuous activity.
The scar will never completely fade. Depending on the patient, the scar may become thinner and less noticeable over time; other patients may develop thicker, more palpable scars. For this reason, be certain to discuss scarring potential during the preoperative interview.
An injection of cortisone may be necessary if the patient shows a hypertrophic scar. In my experience, the scar is more likely to become thinner and less noticeable over time.
After arm-reduction surgery, it is essential to monitor hemostasis, because there is more chance of hematoma development in areas subject to frequent use. A hematoma will interfere with healing and could even result in necrosis of the skin.
The body has ideal proportions, and the arm is a key part of that silhouette. In many warm climates, the upper arms are consistently exposed. Therefore, it is important to restore the proportions of the upper arms relative to the rest of the body.
Patients who have undergone massive weight loss often have hanging skin in their upper arms and, despite their weight loss, they look heavier than they actually are because their arms are disproportionately large. Brachioplasty, therefore, can add to their quality of life and self-esteem.
The surgeon must rely on experience and take the body–arm proportions of patients into consideration to make good surgical judgments. When the surgery has been performed the right way, the surgeon will have achieved an attractive contour that pleases both the patient and the practitioner. There is consistently high patient satisfaction with this type of brachioplasty, particularly in patients who have undergone massive weight-loss surgery.
Mordcai Blau, MD, is a board-certified plastic surgeon in private practice in White Plains, NY. He can be reached at (914)-428-4700 or via his Web site, www.cosmetic-md.com.
Reference
- American Society for Aesthetic Plastic Surgery. Cosmetic Surgery National Data Bank 2006 Statistics. Available at: http://www.surgery.org/download/2006stats.pdf. Accessed March 14, 2007.


